Frozen Shoulder
Written by Mr Simon Boyle, Consultant Shoulder Orthopaedic Surgeon

What are the symptoms with a frozen shoulder?
This starts with a gradual build-up of discomfort and pain in the shoulder. This is made worse by movement, especially when the arm is twisted away from the body or lifted away to your side.
As time goes on, the shoulder becomes progressively stiffer such that activities involving performing overhead movements or reaching backwards becomes more and more difficult. At this stage, sudden unexpected movements of the shoulder can be very uncomfortable. The symptoms from a frozen shoulder can last from several months to 3-4 years without treatment.
What is a frozen shoulder?
A frozen shoulder is a condition where the soft tissues (capsule and ligaments) that support and stabilise the shoulder become inflamed and tightened. The inflammation leads to pain and the tightening leads to stiffness and loss of movement. Another name for a frozen shoulder is Adhesive Capsulitis.
What causes frozen shoulder?
In the majority of cases a frozen shoulder occurs for no obvious reason (idiopathic), although they seem to occur more frequently in females between the ages of 30 to 60. In some cases a frozen shoulder comes on after trauma such as a fall, fracture or dislocation. A frozen shoulder happens to 1 in 20 people after shoulder surgery.
Some people are more prone to frozen shoulders than others. These include people with diabetes, thyroid problems or changes in hormone levels.
What treatment can be offered?
It is important that a frozen shoulder is diagnosed early as the treatment differs from other shoulder conditions. It is imperative to try and keep the shoulder as pain free as possible and to avoid very painful stretching exercises.
Our Physiotherapists at Yorkshire Sports Medicine will provide supportive treatment to help maintain your strength and range of movement but to avoid painful exercises. For most people, Physiotherapy and painkillers will be all that is necessary to treat a frozen shoulder.
Are any special tests needed?
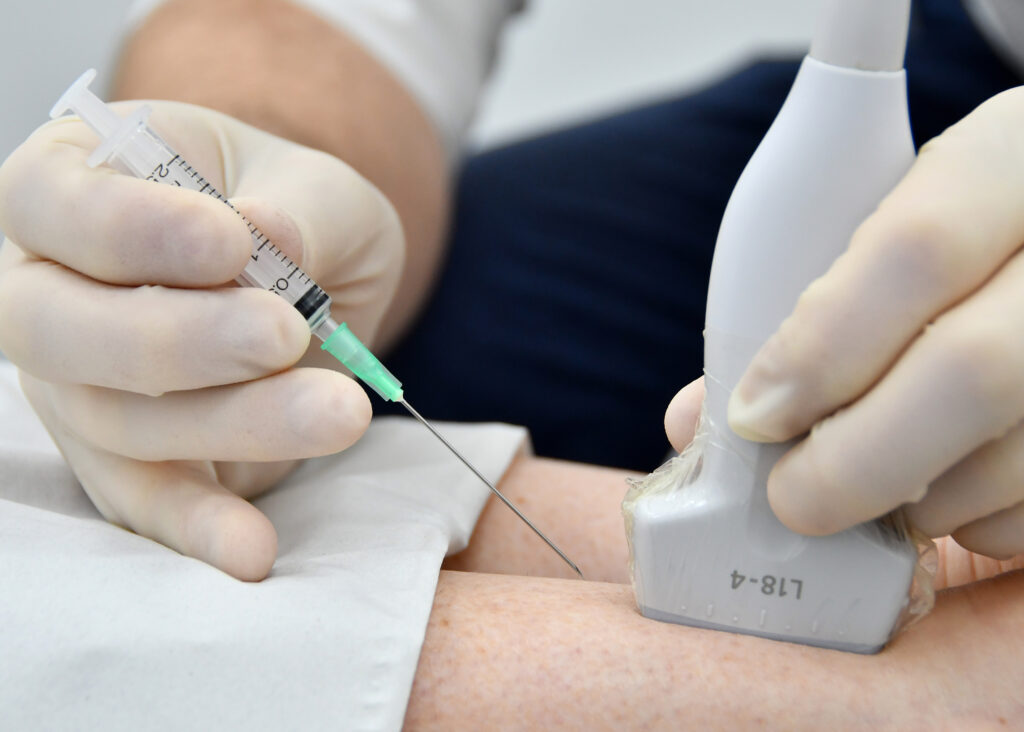
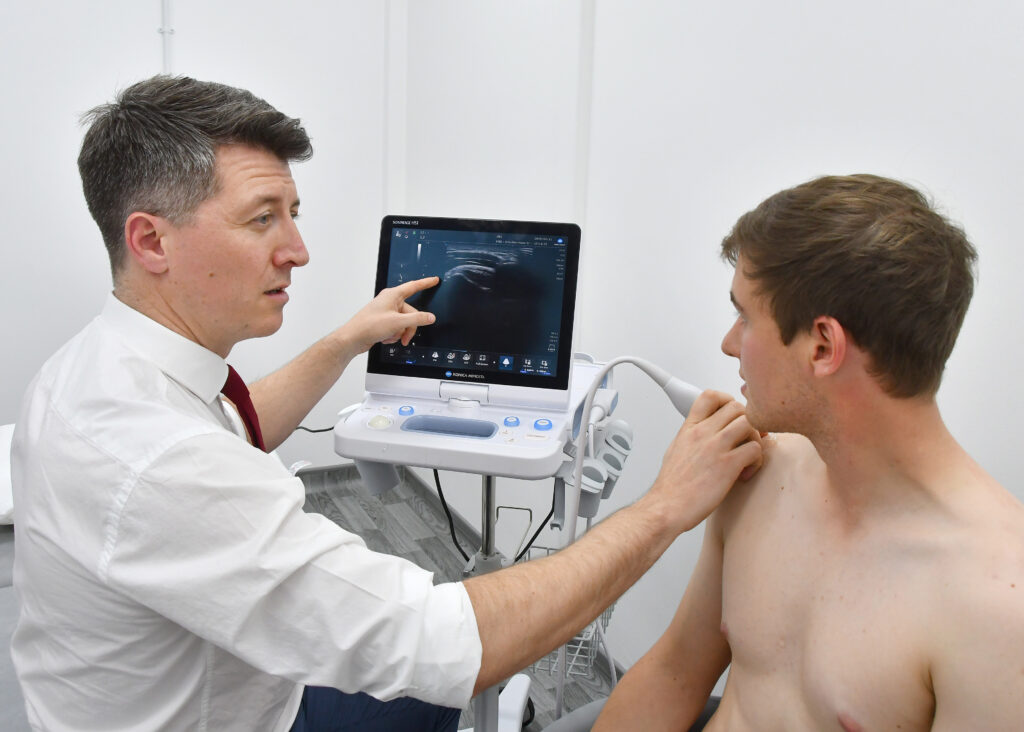
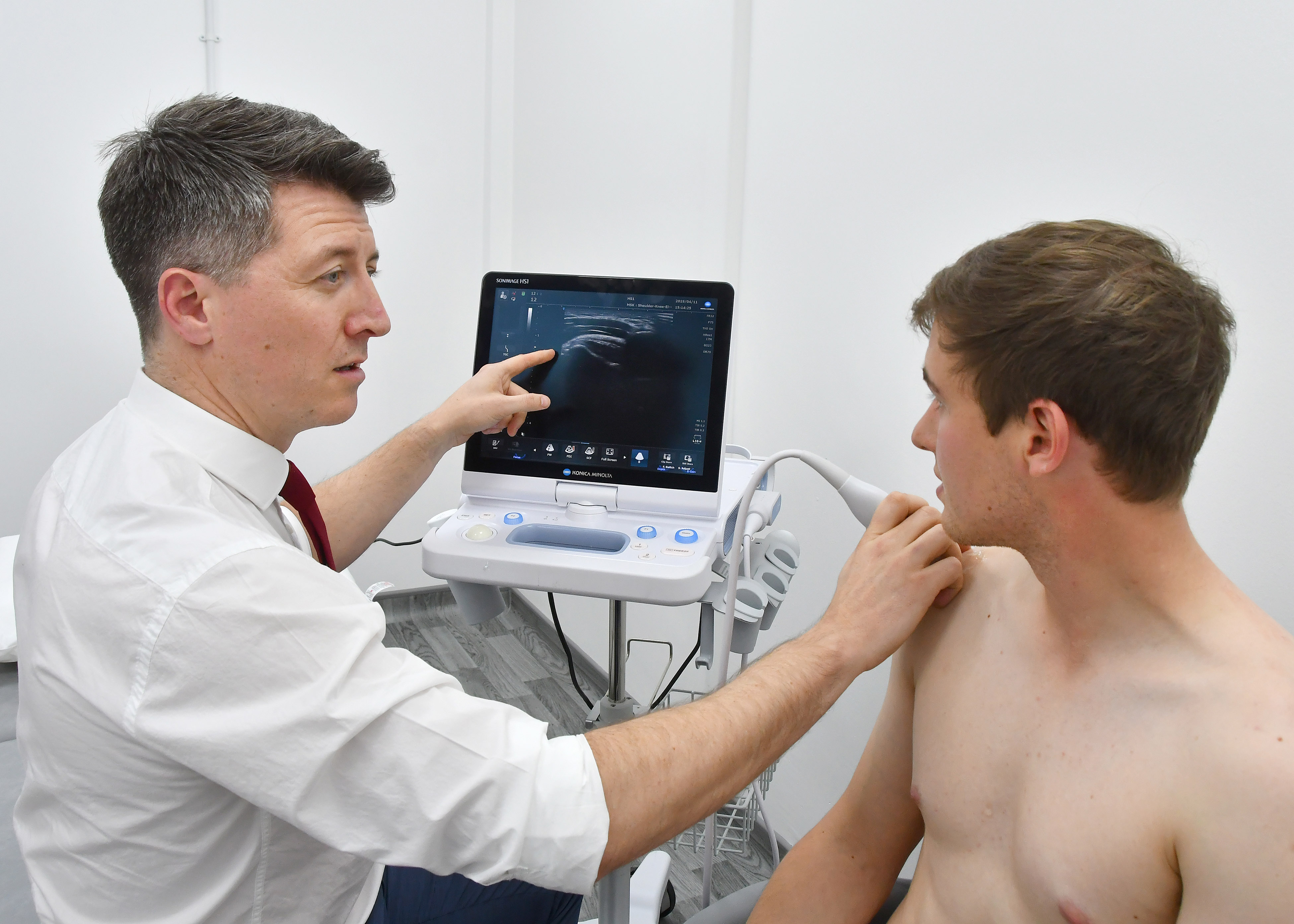
No, however if your symptoms came on as a result of trauma and/or should your symptoms fail to settle despite Physiotherapy, then X-Rays and ultrasound/MRI scans provide good additional information to enhance your recovery. We can perform Ultrasounds at our state of the art facilities and we work closely with our partners to facilitate these scans ASAP. Imaging can be used to detect inflammation, bone spurs or even tendon tears.
What other treatments are available?
Injections – these most commonly take the form of a steroid and local anaesthetic injection. These offer good pain relief and can take effect fairly quickly and last several weeks to months.Side effects of steroids are uncommon but can include:
- the injection not having any pain relieving benefit.
- damage to the rotator cuff tendons (especially if too many are administered).
- infection and post injection flare of symptoms (lasting 2-3 days in approx 5% of cases).
The risks and complications of injections will be discussed with you by your treating Clinician at YSM.
Hydro-dilatation – this is a special form of injection performed under image guidance to ensure the injection is placed optimally (x-ray or ultrasound). It uses a larger volume of fluid than a normal injection to help stretch the tight shoulder joint capsule. This is undertaken to help improve the range of movement as well as providing pain relief. YSM works with our partners and we are able to facilitate timely specialised injections which can be arranged through the Clinic. It is essential to follow this up with Physiotherapy within several days of the injection to take advantage of the pain relieving effects.
Referral to a Shoulder Surgeon – this is used as a last resort where a frozen shoulder is being resistant to other interventions. Your Surgeon will be able to explain the pros and cons of surgery should you reach this point.